Obstetric Emergencies:
“If you cried here, you’d cry every day”
by Séverine Caluwaerts, OBGYN, MPH

Updated March 1, 2019
MARIAMA*
I had been the gynecologist at MSF’s Gondama Referral Center in Bo, Sierra Leone, for one month when a 16-year-old named Mariama arrived at our clinic sandwiched between her mother and father on a motorcycle. She was heavily pregnant, pale, bleeding, and in a lot of pain.
Two nurses helped her off the motorcycle and put her on a stretcher. One inserted an IV line while I palpated her abdomen and asked her family what had happened.
Four days earlier, they told me, Mariama had gone into labor. Like many women in the developing world, she tried to deliver without the help of a skilled health worker.i She was assisted by a traditional birth attendant (TBA), who came to her home, but things did not go well, and after three days, the family decided to come to the hospital.
MSF teams assisted in 309,454 deliveries in 2018.
It was the rainy season, however, which made a long journey even more difficult. They had to travel the first leg by boat just to reach the motorbike. The entire trip took a full day.
I had worked as an OBGYN in Belgium for ten years but this was my first assignment with MSF, and I had never seen a patient in this state. I didn’t understand why the family would have waited so long to bring Mariama to the hospital.
I came to learn that in this community everyone tries to deliver at home with a TBA. That’s the custom. The problem is that most TBAs are not trained to identify pregnancy-related complications that require emergency care. Even when the complications become glaringly obvious, few families in this part of Sierra Leone—or in most of the country, in fact—can easily access a health facility with personnel trained to deal with such things. That is why pregnant women in trouble often arrived at our hospital in very advanced stages of distress. Some arrived too late to assist. Others never made it at all, dying en route.
I can’t tell you the number of times I saw a patient in Sierra Leone or on subsequent MSF assignments and thought: “If only I could have seen this woman just a few hours or a day earlier, this disaster would not have happened.”
Every day, in fact, about 810 women around the world die from causes related to pregnancy and childbirth.ii The majority bleed to death, succumb to severe infection, fall victim to a sudden spike in blood pressure (pre-eclampsia), or die after seeking an unsafe abortion. These deaths could easily be prevented with treatment that is not terribly complicated, if trained medical personnel and proper medical materials are accessible.
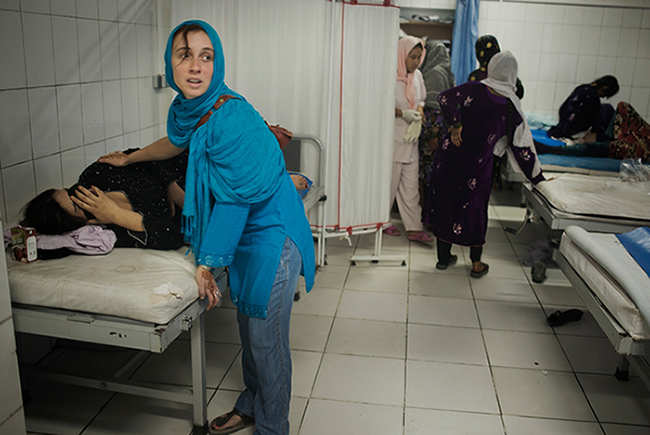
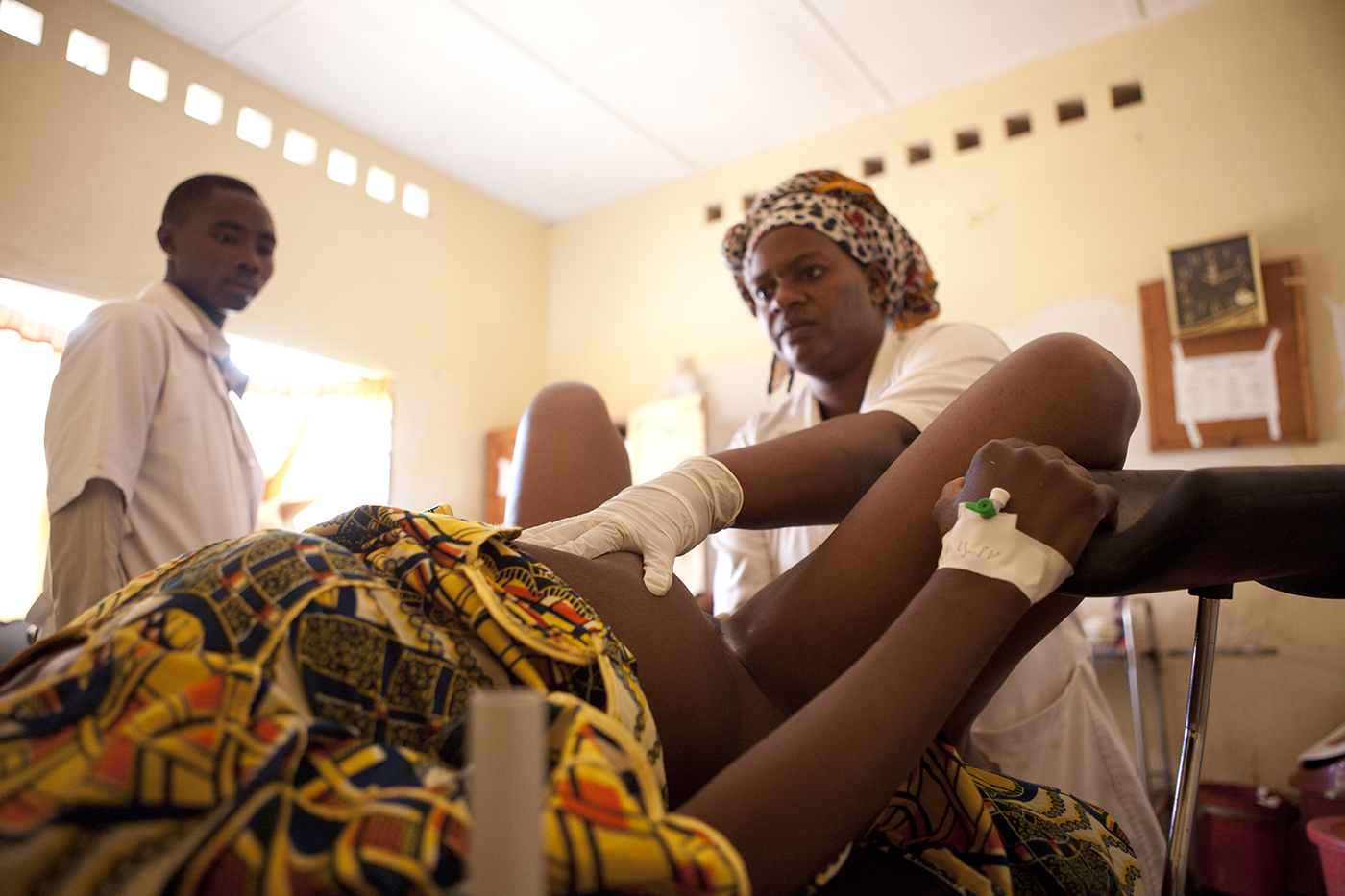
An MSF midwife helps a woman in labor In Kabul, Afghanistan. Photo by Andrea Bruce/Noor Images
But in too many places it is not available, which is why MSF makes obstetric care a priority—in 2018 we ran 123 projects with dedicated emergency obstetric services in places where national health systems are non-existent or have been severely affected by conflict or neglect. Obstetric care is also incorporated into nearly all MSF projects in conflict settings and other situations where large numbers of people have been cut off from care. Where necessary and feasible, teams provide surgical services as well. And they manage pre- and postnatal complications, along with problems resulting from unsafe abortion and miscarriage.
I have been on more than 20 assignments with MSF in sub-Saharan Africa and Central Asia and seen far too many situations like Mariama’s. The lack of access to emergency obstetric care is a problem that goes far beyond Sierra Leone, but Sierra Leone has long had one of the highest maternal mortality rates in the world—it had the third-highest rate in 2017 after South Sudan and Chad, with 1,120 deaths for every 100,000 live births.iii It’s no great mystery why: in Bo’s government hospital, for example, there are almost no doctors, nurses, drugs, and hygiene.
“My daughters and my daughters-in-law deliver at home most of the time. If there are complications, they will go to MSF’s Ahmad Shah Baba Hospital (in Kabul). My daughter just delivered a baby 15 days ago at the hospital. She felt such pain and she was very weak. We sent her by taxi. The transport fare was 200 afghanis [$3.50]. But when she arrived to the hospital she was not ready to deliver and she was sent back home. [Note: MSF’s hospital operates at full capacity every day and can only accept women ready to deliver.] A few hours later, at midnight, she was ready to give birth and had to go to the hospital again, but we didn’t have a car to send her. We knocked on the doors of our neighbors’ homes because some of the families have cars. And finally we found someone to bring her to the hospital. It was not easy.”
It’s heartbreaking. And our job is to assist those we can. In Mariama’s case, we were quite certain that her uterus had ruptured during her prolonged labor. After the nurses and I rushed her into the operating room, I used a mixture of English and the local language, Krio, to explain to her parents that this was serious, that the baby was probably dead—very few babies survive uterine rupture that occurs outside a hospital—and that I would not remove Mariama’s uterus if at all possible. But I needed their permission to remove it if it was necessary to save her life, I added. Her mother started to cry.
The baby was palpable inside the abdomen and was indeed dead, as the fetal heart monitor confirmed. We performed a midline laparotomy, opening her belly from above her umbilicus towards her pubic bone, and extracted the perfectly formed dead baby by his feet. Then came the effort to repair the rupture of her uterus, which extended all the way into her bladder. Were she still at home, she would have died within hours.
After this difficult surgery and a transfusion of three units of blood, we were able to stabilize Mariama. We had also been able to save her uterus, which is extremely important for a young woman in this context. But she was not clear yet. The baby’s head had been pressing against her pelvic bone for so long that she had sustained a fistula—an opening in the pelvic tissue between her uterus and bladder. While not immediately life threatening, a fistula can cause significant and long-lasting physical and social problems for a woman. The sooner it was diagnosed and repaired, the better. When she was ready, we sent her to the nearby West Africa Fistula Foundation for fistula repair surgery.
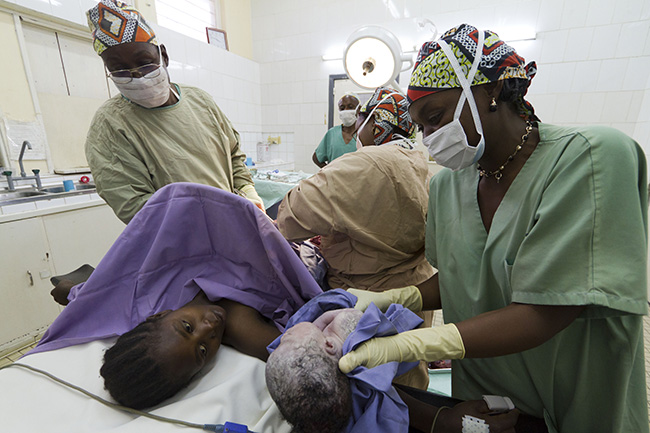
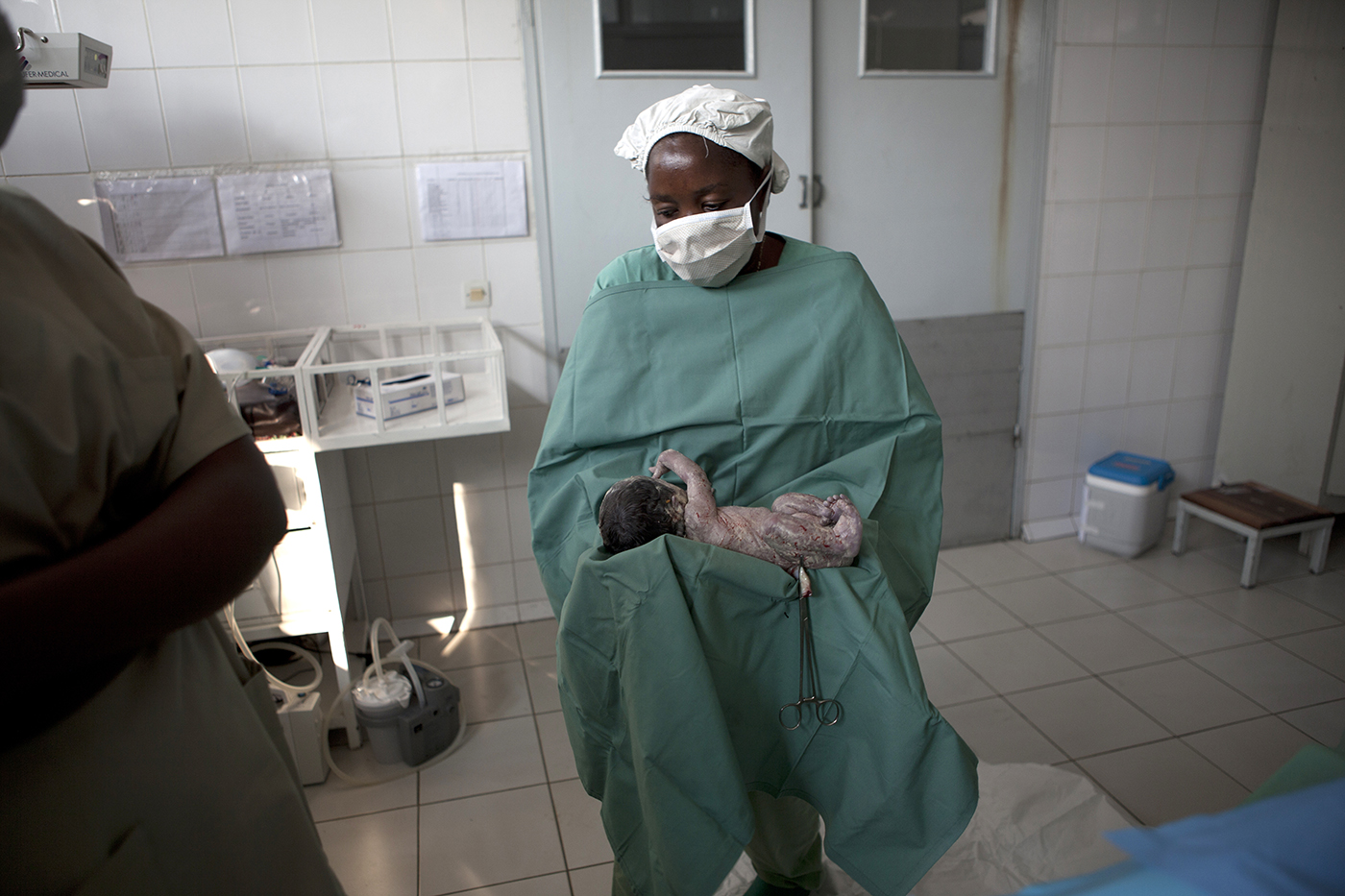
A baby is delivered by C-section to a mother in Rutshuru, Democratic Republic of Congo. Photo by Andre Quillien/MSF
In my first week in Sierra Leone, I performed four Caesarean sections in a row, all on pregnant women who came to the hospital long after they began experiencing serious complications. None of their babies survived; two died before the mother reached the hospital. In Belgium, I’d likely have tears in my eyes if a mother delivered a dead baby, in part because it happens so rarely. In Sierra Leone, I cried in the beginning, too. But it eventually became impossible to cry over every time—not because it wasn’t just as tragic, but because I’d have been crying every day.
I was grateful when I performed a fifth Caesarean and out came a healthy little girl, alive and well. After the surgery, I took her in my arms and she started sucking on my finger, looking for milk. I looked at this beautiful, perfect baby and smiled in sheer relief.
Once, a mother arrived in labor, trying to deliver twins. She was from Bonthe Island— two days travel from the MSF hospital. Two men had carried her part of the way. Then she rode in a boat, then a private taxi. She urgently needed a Caesarean so we put her on the operating table right away.
The first of the twins was positioned with his chin, rather than the back of his head, pointing downwards. It was extremely difficult to extract him because he was stuck in the mother’s pelvis, and when he came out he was not breathing. Our pediatrician tried to resuscitate him, to no avail. Luckily, the second twin was still breathing and was delivered successfully. That was a relief but it was gutting to think that the first twin died solely because his mother could not access transportation to the hospital in time.
[Taken two days after Rosaline’s daughter-in-law was admitted with post-partum hemorrhage to MSF’s Gondama Referral Hospital in Bo.] “At about 9 o’clock on Friday evening I was asleep when [my daughter-in-law] woke me. When I got up she said she was really feeling pain and could not bear it, so I took her to the government hospital. There was no nurse there during the night, so we slept and at 1 p.m. the next day she gave birth. After that she was bleeding, bleeding, bleeding. The doctor told us we could either take her to Freetown, or Mageni, or to Gondama hospital.
Straight away the nurses told us to go to the MSF hospital in Gondama. Luckily we have a car. She needed blood but we could not find anyone to donate. It was very late, so the staff found her two units of blood. If they had not, she would have died. I’m telling you the truth.
They told me that they do everything for the patient except provide blood—the family has to find blood themselves. If you come with people who donate it’s OK. But if there is no one, the staff will try to find blood for you. And, indeed, they did for me. Right now we are still scrambling for more blood.
Parents have to go out by all possible means to find the blood. This morning I went as far as the junction. There I met some boys and we came back here together. Unfortunately, the boys’ blood types did not match with my daughter-in-law. When my husband came with his brother, they also helped and we found someone who matched her blood type. We still need one more pint.”
This is something I saw in numerous other locations where I worked, including in Khost, Afghanistan. There, insecurity in the surrounding area prevented us from getting out on the roads ourselves, but in some places we are able to help bring women closer to care. In the Bo district of Sierra Leone and the Kabezi district of Burundi we started an ambulance service where a nurse or midwife accompanies the patient from a local clinic to MSF’s hospital, giving her the drugs and fluids she needs during transportation. As a result of this system and the quality of care we provided, maternal mortality went down 61 percent in Bo and 74 percent in Kabezi between the late 1990s and 2012.iv It is hard proof of what can be done and how many lives can be saved with some relatively simple efforts.
ZOHRA
During one of my assignments at MSF’s maternity hospital in Khost, Afghanistan, a pregnant woman named Zohra came in. She was 34 and had already given birth to 11 children, nine of whom were still alive. When she got to the hospital, she was already bleeding profusely.
At that point in her life, Zohra had known that getting pregnant again was a health risk. But contraception in Afghanistan is difficult to obtain outside of the capital (and even in Kabul, it’s not simple). Many women in Afghanistan live almost all of their lives at home, with no income of their own and little or no access to family planning. When the Taliban was in power, family planning was explicitly forbidden, and religious opposition to contraception runs deep to this day.
This has serious consequences. The Guttmacher Institute reports that providing contraceptive services to all women who need them has the potential to reduce maternal mortality by about 25 percent, in large part by giving women more autonomy over their own bodies.v Yet access to contraception, including condoms, is very limited for many women for societal and financial reasons. The family planning services that are available where MSF works usually focus on postnatal birth spacing, and staff at the facilities often disapprove of sex outside of marriage. Many young women are alone when it comes to preventing and dealing with unwanted pregnancy. That is why providing contraceptives upon request to women and girls of reproductive age is an important component of MSF’s efforts to prevent maternal mortality.
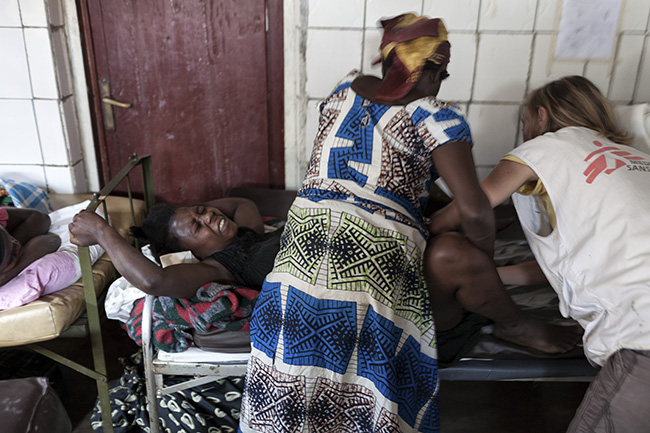
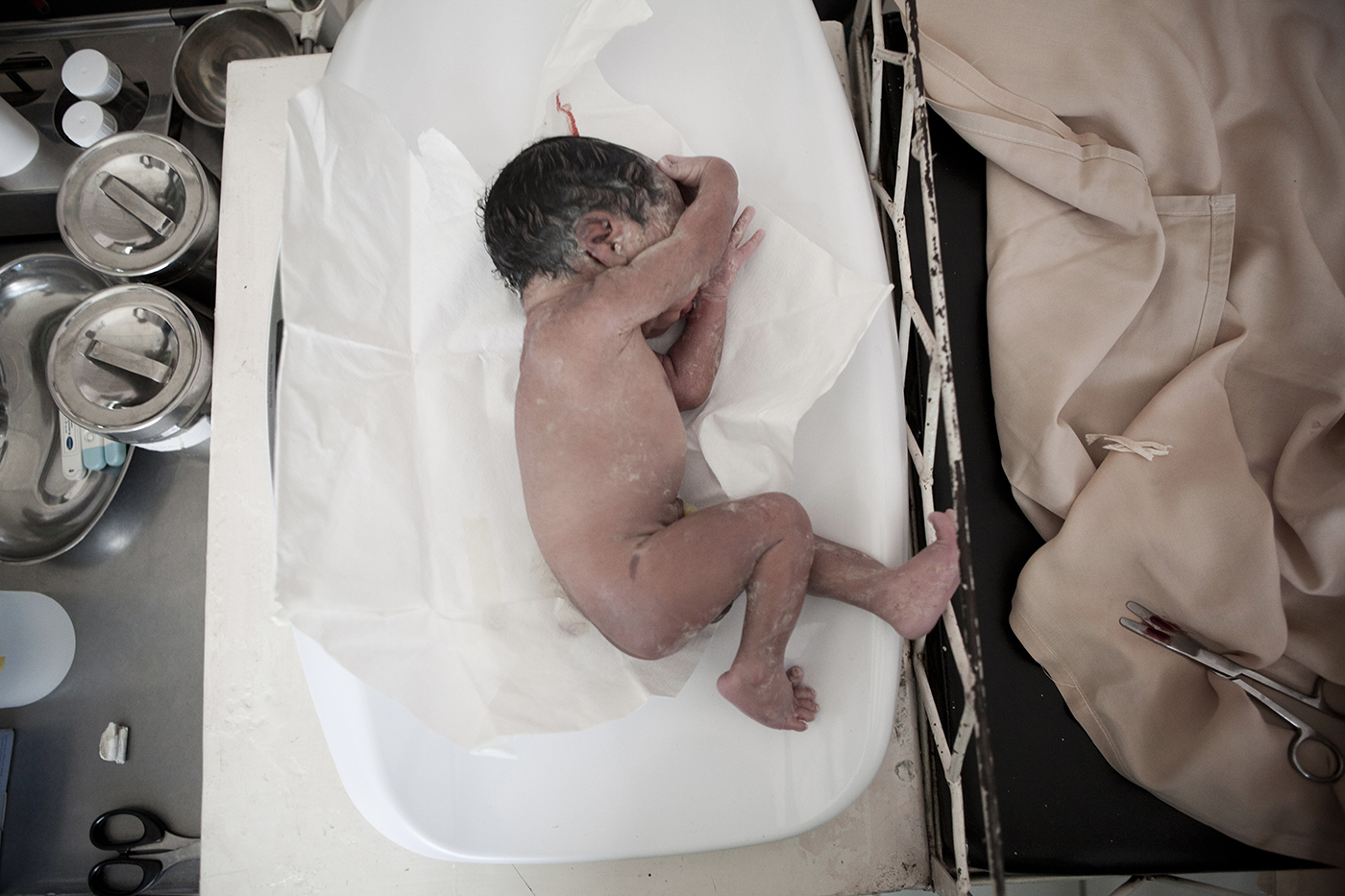
An MSF midwife delivers a baby at a small referral health center in rural Democratic Republic of Congo. Photo by Yasuyoshi Chiba/Duckrabbit
Before opening the hospital in Khost, MSF had arranged meetings with the religious leaders in the area and held several gatherings with community elders. What we heard gave us hope. Many of the community leaders had seen or heard about women dying in childbirth and they wanted to save their wives and daughters from the same fate, so they were very much in favor of MSF opening a women’s hospital. They even allowed us to provide contraception, in the form of birth control pills and injections.
Zohra’s case illustrated in fine relief the need for MSF’s emergency obstetric services. Women like her who have borne many children face two main threats: first, repeated pregnancies stretch the muscle of the uterus to the point that it cannot contract adequately and thus cannot prevent dangerous, heavy bleeding. What’s more, the muscle of the uterus may no longer be strong enough to move the baby into a good birthing position, making it more likely that a woman will have a complicated delivery. In addition, in women who have had previous Caesareans and those who have had several previous births, the placenta can attach to the uterine wall in an abnormal place and obstruct delivery. The potential consequences of each of these factors include severe hemorrhaging, uterine rupture, and death.
Before reaching us, she had made two prenatal care visits to a government-run clinic in her village. She’d also had two previous episodes of bleeding during this pregnancy. Still, Zohra assumed she would have her baby at home. That’s how she’d delivered her previous children, after all. And it wasn’t crazy to think doing so could be safer.
In Afghanistan, there are major difficulties with a hospital delivery. To start, the ongoing conflict can make it very risky to travel to the hospital. Local nurses also told me that some men in rural Afghanistan societies view women as not worth the resources required for a hospital delivery. The hospitals themselves are often under-equipped as well—the clinic Zohra had visited earlier did not have an ultrasound device, for instance.
“This was my third baby. The first two children are also not alive.
When I fall sick in the village I usually come to the hospital, but it is very far. It can take one day on foot to come to the town because there is no health center nearby. I was brought to the hospital today by bicycle because I tried to deliver at home and the baby didn’t come out. It took two and a half hours to arrive here by bicycle.
The labor pain came during the night, around 10 p.m., and lasted into the morning. My family had called the traditional birth attendant. She tried to help me but failed. Around 11 a.m., when we saw the baby was not going to come out, I came to the hospital. It was my uncle who decided I should go.
When I arrived here today the midwife tried to have me deliver vaginally but I was not wide enough, so they cut [The staff performed an episiotomy] in order for the child to be delivered.
With my two first children, when I tried to deliver at home, it happened the same way. There was no doctor so the babies died. When it looked as if it were going to happen again, I wanted to come to the hospital because I didn’t want the same thing to happen, but it did. I was too late. All three have been stillborn.
It happens to other women in the village, too, because we don’t have a health facility nearby. The only thing that would help is if we had health care near us. If a mother needed to deliver she could go to the nearest hospital before she suffered a long, difficult labor. So that is the only solution. But with no health facility, I think the same cases will happen again.”
By the time she reached us, Zohra had been bleeding heavily for two or three hours. Her baby was still alive, however. Through ultrasound we diagnosed placenta previa—the placenta was attached too low on the uterine wall, obscuring the opening to the cervix. This makes it impossible for the baby to move into the birth canal. What’s more, every time the mother has a contraction, the baby pushes on the placenta. This is why Zohra was bleeding heavily.
We took her to the operating room and performed a Caesarean section. Her baby, a boy, survived, but Zohra’s uterus did not contract as we’d hoped it would. She continued bleeding during surgery, and we needed to perform a postpartum hysterectomy—removing the uterus to stop the bleeding and save her life.
Zohra also arrived in Khost at night, desperate for assistance.
In many government-run facilities with staff shortages,
patients arriving overnight often are not seen until the morning.
If MSF had not been there, Zohra most likely would not have gotten the Caesarean, let alone the hysterectomy. Her family was extremely poor and couldn’t afford the cost of such a procedure in a government hospital. Zohra also arrived in Khost at night, desperate for assistance. In many government-run facilities with staff shortages, patients arriving overnight often are not seen until the morning.
Zohra needed four units of blood right away. They were difficult to get. We had to convince the family to summon men to donate blood, which was tricky both because of a cultural resistance to giving blood and the fact that no one wanted to drive to the hospital at night due to the conflict. I spent 30 minutes talking to her husband outside in the freezing Afghanistan winter, explaining how dire Zohra’s situation was. He eventually agreed to call other family members to donate blood for his wife.
The issues around blood go beyond Afghanistan. In Sierra Leone, Mariama had likewise needed donated blood—three units in her case. Her parents were willing to donate for her, but it was often a struggle in that country as well. There were all sorts of rumors about blood donation; I heard, for instance, that you drop dead the fifth day after donating or that it causes sexual impotence in men. I even heard people say they would not donate blood because MSF was selling it for a profit. This was nonsense, but I was still shocked.
It’s with these sorts of concerns in mind that MSF tries to organize a blood bank in every hospital where we work. In Sierra Leone, our lab technician organized a one-Saturday-a-month blood donation day. We advertised on the local radio station and offered free food as an enticement. It worked to a degree, but for patients with rare blood groups, finding their types posed many problems. Blood can only be kept in the refrigerator for three weeks, and donations are needed continuously to ensure an emergency supply. In Khost, we eventually got the blood and Zohra recovered without complications. After one week she went back to her family.
RAZIA
It’s not every day that a woman arrives at the hospital having delivered one baby two days earlier and with a second still in the womb, but it happened while I was working in the town of Timurgara in Lower Dir, a mountainous district in northern Pakistan near the Afghan border.
Family members brought Razia by car over narrow, snow-covered roads from Upper Dir. It was January, a time when snow made travel in the area even more laborious than it usually was. Razia was 28. She had given birth to three children previously, but always at home, and that had been the plan again this time. It had never occurred to her husband and family to go to the hospital. Razia had sought antenatal care locally, but no one was able to tell her that she was carrying twins.
After Razia delivered a healthy boy at home, she was stunned to learn that there was another baby inside her. More troubling was the discovery that the baby was in a transverse position, its umbilical cord already out. The family and the traditional birth attendant waited and waited, but the baby did not shift into a good birthing position.
At first, as religious people, they had faith that the problem would be resolved. But as time went on, they realized they needed help. Two days after she first went into labor, Razia’s husband took her to the local clinic, which immediately referred her to MSF’s hospital in Lower Dir. It was a big psychological step for them to leave their village for an unknown town, not knowing what to expect from health services in another region, not to mention driving along treacherous roads in a snowstorm in a war zone. But they were willing to go.
“Some patients come to MSF’s hospital in Khost from far away and they cannot travel during the night due to security issues. Some patients have told us they were not able to come to the hospital when there was shooting and fighting, even though they were in labor or bleeding. Instead, they went to the nearby health centers. But some public health centers only have staff working in the morning.
There are also private clinics that will induce the patients when they are not yet in labor, and sometimes the baby or the mother dies. Uterine rupture and obstructed labor are common. Many patients come to our hospital after having been induced in the private clinics. They come when they have complications, such as fetal distress. It happens a lot.
The patients come to MSF because we have free medical care. In the public hospital if patients need a Caesarean section, they have to buy the medicines themselves from the bazaar, including the antibiotics needed after the C-section.
Women also come because we only have female medical staff. Even if a woman is at risk of dying, she doesn’t want to be examined by a man. Of course, there are not many female doctors in Khost. We have seven female doctors in the whole province. One of them is working with MSF.”
At the time, MSF was not organizing transport at night because of poor security, so Razia’s family had to find their own way to the hospital. They arrived at two in the morning. Razia was stable and alert. To my surprise, the baby was still alive and its heartbeat was strong and regular. I performed an emergency Caesarean section and a screaming, healthy little girl was delivered. Our operating staff called her “a miracle of Allah.”
Razia recovered quickly and was determined to get back on her feet the day after her surgery so that she could care for her new babies, and she left the hospital after five days. Before she departed, we offered her contraception, which would enable her to wait at least two years before her next pregnancy. She declined. Her two eldest children were girls, and she only had one live boy. There is a strong preference for boys in Pashtun culture, and she was hoping to have another boy soon. If she did not produce one, she worried she would not count in the eyes of her husband and her mother-in-law.
Razia and her baby girl were very lucky. The nurse in their local health care center knew about the MSF hospital. The MSF team upon arrival had organized meetings with the community in Timurgara to let people know that MSF provided lifesaving care 24 hours a day, seven days a week. But Razia was not out of danger. She now had a Caesarean scar, which put her at higher risk of complications during her next pregnancy. There were medical reasons that she should wait two years before getting pregnant, as we informed her. The scar may not be completely healed by the next time she tries to deliver.
Governments must recognize the need to provide emergency obstetric care
for their citizens, and if they can’t, for whatever reason,
the international community must try to step in and provide those services.
I told her that if she became pregnant again, she would need to deliver in hospital. I’m sure she heard the message, which our local nurse translated to Pashtu. But I’m not sure she will follow our advice or that her husband will let her deliver in hospital, short of the emergency situation that brought her to us in the first place. If she did get pregnant again, I’d be worried about a possible uterine rupture, especially because she lives in a remote area, far from health care. This is why in places where there are few opportunities for a pregnant woman to find surgical care, MSF will only perform a Caesarean section on a patient whose life is at risk.
What strikes me about Razia’s story, and that of Mariama and Zohra, is that I will never know what happened next for them. We met them at a moment of crisis, we solved a life-threatening problem, gave them advice for the future, then let them go. But anything can happen once they leave the hospital, and we can never count on them coming back, or being allowed to come back, the next time they need medical help.
If women in developing countries had accessible obstetric care in their communities, I wouldn’t have to worry about Razia, Mariama, Zohra, and the hundreds of women I’ve treated over the years. Eight hundred women would not die every day while we know how to save them. It is tragic that in many parts of the world today, women have no access to quality obstetric care administered by properly trained staff.
Governments must recognize the need to provide emergency obstetric care for their citizens, and if they can’t, for whatever reason, the international community must try to step in and provide those services. Even in conflict settings—especially in conflict settings—we have to find a way to attract doctors, nurses and midwives, and to make services available 24 hours a day, seven days a week, and to make transportation available as well.
Many nongovernmental organizations lack the capacity to provide hospital services and big donors—donor countries and organizations—are often reluctant to invest in them. But if we truly want to improve maternal mortality rates, they will have to find a way.
At MSF, we continue working to improve our quality of care in obstetrics, dedicating some programs exclusively to emergency obstetric care and integrating it in all our programs. We urge others in the international medical field and local health authorities to put the needs of pregnant women and their unborn children at the forefront of their programming. There are 810 lives (at least) at stake every day.
*Patient names have been changed.
iUNICEF, “Global Delivery Care Coverage and Trends, Percentage of births assisted by a skilled birth attendant, by country, 2013-2018,” April 2019. https://data.unicef.org/topic/maternal-health/delivery-care/
iiWHO, Maternal Mortality Fact Sheet, updated September 2019.
https://www.who.int/news-room/fact-sheets/detail/maternal-mortality
iiiWHO, UNICEF, UNFPA, The World Bank, and the United Nations Population Division, Trends in Maternal Mortality, 2000-2017, World Health Organization, 2019. https://data.unicef.org/resources/trends-maternal-mortality-2000-2017/
ivMSF,“Safe Delivery: Reducing Maternal Mortality in Sierra Leone and Burundi,” November 2012. http://reliefweb.int/sites/reliefweb.int/files/resources/MSF%20Safe%20Delivery%20ENG.pdf
vGuttmacher Institute, “Adding It Up: Investing in Contraception and Maternal and Newborn Health, 2017,” December, 2017. https://www.guttmacher.org/fact-sheet/adding-it-up-contraception-mnh-2017#figure4