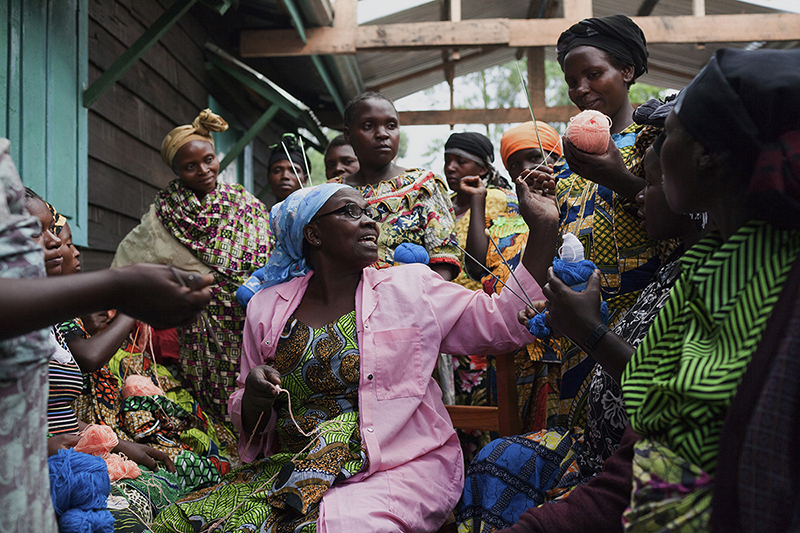Maternal Health Before
and After Childbirth

The Lead-Up To Birth: Essential Antenatal Care
By Nele Segers, Midwife, with Olivia Hill, RN, RM, BSc, MSc, and Eva Deplecker, Midwife
One morning in Gogrial, South Sudan, Grace* arrived in our emergency room with her newborn baby. She was worried because he was sick and refusing to take her breast milk. When we examined the baby we found that he had tetanus, a disease both common and dangerous for newborns that is caused by exposure to a deadly bacterium.
Hundreds of thousands of babies die every year from neonatal tetanus, many in rural areas where it’s very difficult to practice good hygiene. These babies might have been delivered by someone with dirty hands, or their umbilical cords might have been cut with a dirty razor or knife, or they might have been dressed with unclean material.Tetanus has no cure, but it is preventable, and all women of childbearing age should receive vaccinations for the disease. This is a standard part of antenatal care (ANC). The vaccine protects the mother and the mother’s tetanus antibodies, once transferred to her baby, protect her child, too.
When we asked Grace if she had received her tetanus vaccination as part of her ANC, though, she replied that she had never had any ANC at all. The odds of her newborn surviving were not very good. Somewhere between 10 and 60 percent of babies with tetanus will survive if they get hospital care. One hundred percent of babies with tetanus will die if they do not get hospital care.

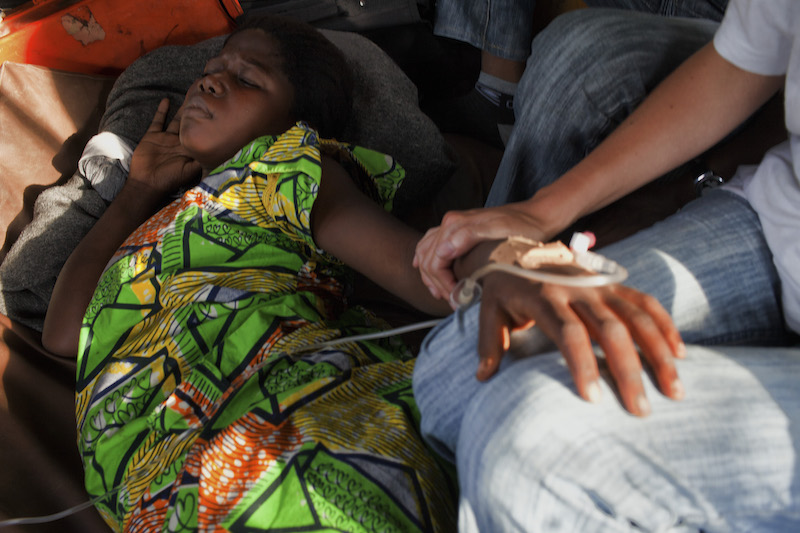
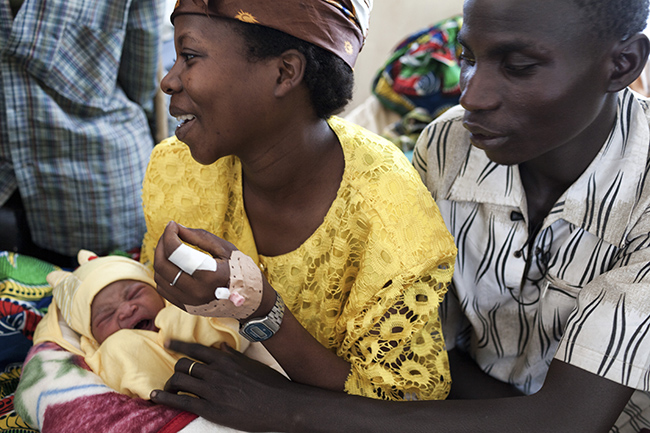
In Burundi, one of the countries with the highest rates on maternal mortality, women are often a long way from the nearest health facility. Photo by Matteo Bianchi Fasani
MSF offers reproductive health care in more than one-third of our projects, and ANC is part of the package. Many government health systems in developing countries offer the service as well. But in too many places, expectant mothers either cannot access it or do not fully take advantage of it. That was what happened in Grace’s case, and now, because she had not gotten ANC and the tetanus vaccination offered as part of it, her baby’s life was hanging in the balance.
We admitted Grace’s boy and administered antibiotics, but he was not doing well. To nourish him, we ran a tube through his nose into his stomach. I explained to Grace and her husband that she and the baby needed to stay at the MSF hospital. The baby was running an extremely high fever and standard procedures were not lowering it. As a last resort, we cooled the baby with ice. Under most circumstances, there’s no way I would do this, but nothing else had been effective. Luckily, the ice worked. The baby’s fever abated, and he gradually recovered from tetanus.
Later, the parents agreed to do a videotaped interview, something we could then use to convince other pregnant women to come in for at least two ANC visits before they delivered. We stressed the two visits because the tetanus vaccine must be given to an unimmunized woman in two doses, usually during the first and second ANC visits. I hoped that a local husband and wife speaking in their own language could better communicate why couples should come in for ANC when they were expecting a child.
During ANC visits, midwives can talk with the mother,
about her birth plan. Where will she deliver? How will she get there?
What transportation will she use? Will she have money for it?
Grace, her husband, her sister, and another family member all participated enthusiastically. Their experience had left them convinced about the need for ANC. At the end, her husband declared, “Next time I will even force her to sit on the back of my bicycle while I take her the 35 kilometers to the center—twice!—so that she will have the tetanus vaccine!”
When MSF opens a new project in an emergency, such as a conflict or natural disaster, we make the provision of obstetric care a priority. The team also provides basic ANC services to all pregnant women. This includes performing basic examinations, identifying potential complications, offering nutritional supplements, advising mothers on the benefits of delivering in a health facility, providing tetanus vaccinations and working to prevent or treat anemia and malaria—since malaria, which is endemic in many places MSF works, can cause pregnant women to give birth prematurely.
“I am having some contractions now. I want more contractions. I asked the midwife here to give me an injection for more contractions, but she said MSF would not give this to me. I want to end this problem. I have leg pain. [The pregnancy] is too heavy for me.
[Patients in labor in Afghanistan and Pakistan frequently ask for injections of Oxytocin in order to deliver faster. The drug is safe if it is administered to a patient with a medical need for it through infusion, with the dosage gradually increased. However, misused injections of oxytocin are dangerous. They can cause uterine rupture and the baby can die.]
When I delivered in private clinics previously, they gave me injections to induce the contractions, but MSF doctors told me the injection is not good for my health. Now I know and I don’t go to private clinics for an injection.
I have done two antenatal checkups for this pregnancy. My tummy was too big so I went for antenatal care. I didn’t know it was twins. If my stomach was not this big, I would not have gone for a checkup. In my village, women usually don’t go for antenatal care.
The road here was okay, but I will not travel after 8 p.m. There are robbers and they stop the cars and steal money. Even if we need to go to the hospital during the night, we will not go; we will wait until at least 5 a.m. to travel.
Sometimes the road is blocked because of the fighting between the armed forces and opposition groups. It usually happens during the night. We hear shootings sometimes, and we will stay at home if there is shooting.”
Once a team has established a baseline level of care, they will add more services as quickly as they can. The World Health Organization recommends that women have at least four ANC visits during each pregnancy, one visit in the first trimester of pregnancy, one in the second, and two more during the third.
During the visits, a midwife should also test and treat the mother for anemia, malnutrition, sexually transmitted infections, HIV, and hypertension (high blood pressure)—whichever that apply. Blood pressure is a key area of focus, since it can lead to pre-eclampsia and then eclampsia, a severe constellation of problems that can threaten the lives of the fetus and the mother. Along with obstructed labor, infections, severe bleeding and unsafe abortion, eclampsia is one of the five main causes of maternal mortality.
One reason ANC is such a crucial part of the effort to reduce maternal and newborn morbidity and mortality is that it connects women to the idea of delivering in a health facility. During ANC visits, midwives can talk with the mother about her birth plan. Where will she deliver? How will she get there? What transportation will she use? Will she have money for it? What happens if something goes wrong?
Ideally, as part of this conversation, midwives can convince women that their best and safest option would be to deliver at a hospital that has trained attendants and can handle serious complications, should they arise. But if a woman insists on delivering at home, the midwife then needs to tell her how to recognize danger signs, so she knows at what point she should be sure to seek out emergency care.

An MSF nurse helps a woman give birth in a field in Burundi. Many times women try to come to a health facility but
they are delayed by distance, access to transportation, conflict, or fees they cannot afford. Sometimes they don’t
have the power to decide to go themselves. Photo by Matteo Bianchi Fasani
In developed countries, many women make far more than four ANC visits, but they have options that people in places with limited to non-existant health systems do not. The WHO reports that between 2006 and 2013 only 38 percent of pregnant women in low-income countries made at least four antenatal care visits.i That rate will be even lower in more isolated rural areas like Gogrial.
One reason for this is a sense that preventative care—going in for treatment before something is evidently wrong—is not part of customary health seeking behavior in many places. Basic needs such as finding food or water or firewood seem far more pressing. What’s more, if they do make the journey to a health facility, which by itself can take up half a day or more, they may have to spend hours at the facility, which might not seem worthwhile.
MSF tries to persuade more women to come for ANC by offering incentives such as mosquito nets or soap, which are important for their families’ health. Where possible, MSF runs mobile clinics to outlying villages for ANC visits, bringing the care to the communities, but MSF teams can only cover limited areas. There are always women further afield who are beyond the teams’ reach.
On average, MSF teams usually see women coming in for between one and two ANC visits, usually late in their pregnancies. MSF has had to adapt to this reality, so staff work to provide the most possible benefit from every visit—since it may be the only time a woman gets any medical care before she delivers.
When women who have not received ANC come in to deliver, MSF health staff run easily administered tests for syphilis, gonorrhea, and HIV, and after birth, will offer counseling and treatment if any of the tests are positive.
Midwives talk about the “three delays”
that can kill a mother in labor or her baby.
The norm for women in many places where MSF works is homebirth, often with the assistance of a traditional birth attendant (TBA). TBAs are highly respected members of their communities who are upholding a tradition that stretches back generations. Those I’ve met have spent decades delivering babies after having apprenticed with their predecessors. They are frequently a pregnant woman’s only connection to maternal care of any kind, and many women prefer the idea of giving birth at home with a TBA to the notion of going to a medical facility.
For women with complications during childbirth, however, TBAs are are not enough. They do not have the skills nor the medical materials to prevent women from dying.
Midwives talk about the “three delays”ii that can kill a mother in labor or her baby. The first stems from an assumption or hope that a TBA is all they need, so they do not seek out any other pre-delivery assistance, and then do not go to a properly resourced medical facility when complications arise. Few would-be mothers can recognize these complications by themselves, and the TBA might not know how to recognize them either. But if the TBA cannot tell that the mother’s placenta is in the wrong place, for example, they’re likely to wait too long before heading to the hospital.

Women wait in line for health care at MSF’s Ahmed Shah Baba Hospital in Kabul, Afghanistan. Over 600 patients
come through the hospital a day for free, high-quality care. Photo by Andrea Bruce/Noor Images
To address this, MSF tries to build relationships with TBAs, so they know what services we offer. We also provide trainings for them on recognizing potential complications. We do not train TBAs to do home deliveries, but MSF sometimes hires them to provide other assistance in our maternity wards. The goal is the same: we want them to bring mothers to our hospitals or to other facilities where they can receive the skilled birth attendance that can mean the difference between life and death.
MSF staff carried out 712,278 antenatal consultations
at 131 projects in 2013.
Working with TBAs can be controversial because many people see them as an obstacle preventing women from getting proper care. Some countries, like Uganda and Sierra Leone, have gone so far as to ban TBAs from practicing at all. Nigeria began regulating the practice of traditional medicine, including TBAs, in the 1970s and started creating model traditional health care clinics with registered care providers.iii
But the fact remains that in many places TBAs are the only option women have, particularly women living in rural areas, far from the resources and hospitals of bigger cities. In Masisi, Democratic Republic of Congo, our ANC team would walk through the bush for hours, three times a week to reach villages that would otherwise have no access to maternal care. The TBAs are often our first point of contact and in many cases they are helpful. But we’re also aware that we’re asking them to send people to us, which means forgoing income they would have made.
The second delay is when a woman cannot reach a place with skilled medical care. It might be too far away. Or there might not be any transportation available, or the roads are too dangerous, or a husband or parent doesn’t think it’s worth spending the amount of money it requires. If a plan has already been worked out during the ANC process, it can pre-empt some of these factors.
The third delay is an absence of good quality care at a health facility. A mother could arrive at night when no skilled staff would be present. There may be staff but no drugs or equipment. In some places where medical care is supposedly free, facilities lack medical materials or even medicines, and the woman has to provide her own. If she can’t provide these often expensive items, she may be ignored, mistreated, or denied admission.
“When the people in our village are sick we go to a private clinic and things are expensive. Drugs are expensive. Consultations are expensive.
I came here to the hospital because of labor pain. I have had the pain for two days. My parents called the traditional birth attendant to come and attend the delivery. The birth attendant stayed with me until the morning. I went to the church to pray, then, after morning prayers, I took public transport to the hospital. We don’t have maternal care in the village.
When I arrived here, the midwife confirmed that I’m in labor, and I delivered.
Whenever I want to come to the hospital it is easy for me to use public transport. I’ve come here for antenatal care during previous pregnancies. I’m not like other mothers because our area is a little bit close to the town.
The best way to help the mothers is to send a health educator into the villages so they will come to the hospital when they fall sick. It is very important.”
MSF and other health care providers have implemented strategies to address the three delays. The most notable one involves bringing women closer to care by offering them the chance to spend their last weeks of pregnancy living in safe, comfortable maternity waiting houses. These have been extremely successful—and some women are even referred by TBAs with whom we’ve established relationships.
In Masisi, the mobile ANC team identifies women who are likely to need emergency care—those with previous Caesarean sections, pre-eclampsia, or several previous births. Nearer to the woman’s birth date, the TBA in her community walks with her to the waiting home, which is located on the grounds of MSF’s hospital. Women receive free food, a bed, and the space to rest in the company of other pregnant women. When it is time to deliver, they do not have far to go to receive skilled care and, if needed, surgical care. The waiting house can receive more than 70 women at a time and it has been in high demand since it opened in 2009.
The MSF team in Aroressa, Ethiopia, saw the same high demand when they opened a maternity waiting home in the isolated, mountainous area where they were working. One woman, Fayza, was near the end of her pregnancy when she was referred by our outreach team to our maternity waiting home. If she had stayed in the mountains where she lived until delivery, the local clinic staff, which lacked trained midwives, may have sent her to the understaffed, undersupplied health center nearby. They could not have brought her by car to our health center. The roads were so bad that we had to use horses, and even they had trouble in the mountains.
Women receive free food, a bed, and the space to rest
in the company of other pregnant women.
When it is time to deliver,
they do not have far to go to receive skilled care.
Because Fayza reached us early enough and stayed in our maternity waiting home, she could give birth in our clinic. In her second stage of labor, her baby’s heartbeat began to sound very faint. We determined that the baby was in fetal distress, but we had the necessary equipment and we delivered him alive. Again, if Fayza had delivered in the mountains, her baby could have died or suffered brain damage from a lack of oxygen during labor. The maternity waiting home—and her decision to stay in it—almost certainly saved her baby’s life.
We had started with just a few rooms because we did not know whether mothers would respond to a maternity waiting home in Aroressa; it can be hard to predict what will be acceptable in a given community. Whereas in Masisi mothers are admitted to the waiting home if they face a high risk of complications, in Ethiopia I had to weigh both the risk of complications and the distance the mother lived from the clinic, because transportation was such a major issue. Still, within one week of establishing this service, we had 20 patients.
We quickly grew from a few rooms to a large tent to an entire house. Maternity waiting homes can be costly to operate, but given the impact, and the lives saved, we were convinced that it was more than worthwhile.
In some regions, particular issues must be addressed: one is female genital mutilation (FGM). There are places where MSF works in which the practice is common and nearly all the pregnant mothers a midwife sees will have undergone some type of FGM.
Usually performed on a girl when she is very young, FGM can lead to many harmful complications in the course of a woman’s life. It is most often during deliveries, however, that MSF deals with problems related to FGM. About 15 percent of all women with FGM have undergone infibulationiv, in which the circumciser narrows a girl’s vaginal opening by cutting and repositioning part of the labia to create a seal. When the girl’s legs are tied together for a period of time the seal fuses.
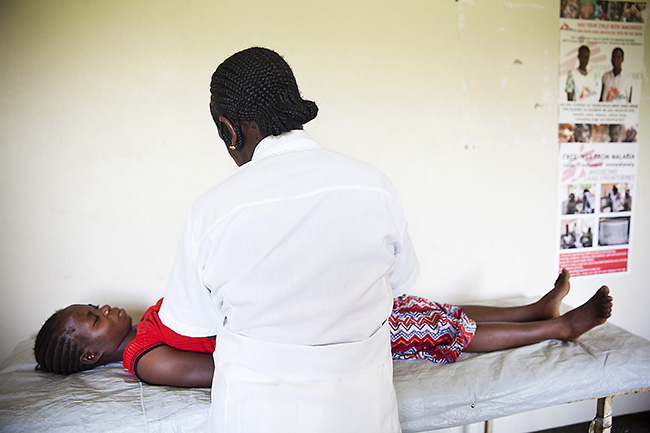
A pregnant woman in Gangura, South Sudan, receives an antenatal consultation from MSF medical staff. Photo by Anna Surinyach/MSF
A woman who has been infibulated may have to be de-infibulated to give birth. If this is performed by an unskilled person in an unclean environment, the de-infibulation can cause obstetric complications that affect mother and baby. Obstructed labor can lead to hemorrhaging in the mother and a lack of oxygen for the baby, which can leave both mother and child traumatized and vulnerable to infection. To avoid such dangers, women with FGM need to be encouraged to deliver in a health facility.
It used to be that ANC was designed to help health workers identify which women were at risk according to certain criteria, and then to decide who needed to deliver in a hospital based on that criteria. However, maternal mortality did not consequently decline, because complications very often cannot be predicted. Many, but not all, problems are preventable with good care, so MSF’s goal is to have all women come to the hospital to deliver—even if they only make one or two ANC visits during their pregnancy.
MSF has adapted its approach to antenatal care to the realities of women’s lives and the competing needs they face in the places where we work. There are some limitations to this approach, some inherent frustrations as well. But there is still much we can do and accomplish. We can establish maternity waiting homes and make sure women in the area know about them. We can connect and form relationships with TBAs. We can give women incentives to come to ANC, we can run mobile medical units, and we can provide testing and counseling during labor. And we do all these things in an effort to ensure that women have the greatest possible access to emergency obstetric care. Insofar as ANC can connect women with these services, it can help save their lives.
The Risk Doesn’t End When the Baby Is Born: The Importance of Postnatal Care
By Debbie Price, CNM, DrPH
A few years ago, I was in central Chad, working in a field hospital that our team had established inside a camp for around 170,000 internally displaced people. I was doing ward rounds in the maternity unit, a standard practice in hospitals where the midwife goes from bed to bed, examining mothers and their babies, making note of who should be seen by the doctor, who needed tests or treatments, who could use extra support with breastfeeding, and who could be discharged that day.
Suddenly, a woman ran into the ward and told us that her neighbor, a woman named Mariyamu, was badly ill. Some team members and I followed her to the neighbor’s hut, where we found Mariyamu lying on a thin mattress, moaning, with her newborn baby lying next to her.
Mariyamu was 17. Days earlier, she had given birth to the baby, her first, inside the hut with the assistance of a traditional birth attendant. Mariyamu’s few belongings—a cooking pot, a jerry can, some plastic plates and cups—were arranged neatly around them, but the young woman was clearly in a state of distress.
We checked the baby, who seemed fine. When I examined Mariyamu, I saw that she was feverish, her lower abdomen was tender, and she was enveloped in a foul odor, which indicated a postnatal infection. Puerperal infection, which is sometimes called “childbed fever,” describes any bacterial infection of the genital tract that occurs after childbirth.
Most commonly caused by the person assisting in the delivery’s failure to wash their hands or otherwise practice good hygiene, it affects about 4.5 percent of all birth mothers, which amounts to roughly six million cases per year.v Another contributing factor is retained tissue—fragments of placenta or bits of membranes from the amniotic sac that did not come out during delivery.
The postnatal period is the most dangerous time
for mother and baby: 75% of all neonatal deaths
and more than 35% of maternal deaths occur in the first week after birth.
Untreated infections, including puerperal sepsis, account for 15 percent of all maternal deaths.vi But when a woman is assisted during delivery by a skilled birth attendant, the risk of infection is reduced by half. A trained midwife knows to make sure anything that touches the baby is clean. When the placenta is delivered, the midwife sees that all the membranes are carefully teased out, and she will check the delivered placenta to make sure it is not missing any fragments. Only 46 percent of births in developing countries, however, are assisted by skilled attendants.vii
We took Mariyamu to our postnatal ward and removed the retained tissue from her uterus. We then started her on antibiotics for her infection and other medication to ease her pain. We examined her baby, Rosalie, more closely, and she was still fine. Mother and child stayed at the hospital for five days, during which time Mariyamu recovered and we helped her establish breastfeeding. When she was healthy, she returned home with Rosalie.
“I gave birth to my third child yesterday—a girl—by Caesarean section. It was my first C-section: my other two children were born naturally at the Kabezi district hospital.
As I was reaching my due date, I was really scared. I could feel that this pregnancy was different from the others.
With the previous two I felt as if my belly was dropping lower as I approached the birth. But for this one, it didn’t—I actually felt as if the baby was moving up into my chest. Also, instead of feeling contractions, I just had terrible pains in my abdomen.
At home, people were trying to reassure me that the pregnancy just hadn’t reached term yet. They said that I should wait, that things would happen naturally. But I really felt things that were not like my previous pregnancies.
And as I’m not used to giving birth at home, I thought it would be better to come here, where there would be people on hand who could help me.
About a week ago, I went to the district hospital to get a consultation as per normal. They told me that I should come here to the MSF hospital. But when I arrived here the staff told me that my pregnancy hadn’t reached term, and that I had to wait a bit.
I really didn’t feel well so I said instead of going home I’d prefer to stay here with the other women in the maternity waiting home. A week passed, and yesterday I gave birth by Caesarean section. [Odette’s labor was obstructed.]
I am feeling a lot better than I did yesterday. Save for the pain of the wound I have from the operation, I feel good. I’ll stay here as long as it takes to get back on my feet then go home.”
The first six weeks following childbirth, the postnatal period, is the most dangerous time for mother and baby. Seventy-five percent of all neonatal deaths occur in the first week of the postnatal period.viii More than 35 percent of maternal deaths occur during this time, too; most, in fact, happen within the first 24 hours.ix The main causes are excessive blood loss/hemorrhage and pregnancy-related high blood pressure (including eclampsia). Those who die in the second to fourth weeks most often succumb to infection. Mariyamu would have been one of those women had she not received help.
One of the major differences between giving birth in developed and undeveloped countries is access to postnatal care (PNC). It stands in contrast to access to antenatal care (ANC), which has been recognized for decades as an important part of maternity care and is often the only component of it that a woman ever receives. Whereas ANC has benefitted from longstanding campaigns in developing countries by the World Health Organization, ministries of health, and non-governmental organizations, the importance of PNC has gotten much less recognition. In 2013, MSF staff conducted roughly one-third as many PNC consultations as ANC consultations.
Over the past few decades, as more and better data have been captured, the medical community has realized that for many pregnant women, life-threatening complications cannot be identified during ANC. They have also seen that many maternal deaths occur in the postnatal period, underscoring the importance of PNC. It was asserted in a 1996 study published in International Journal of Gynecology & Obstetrics that if PNC were provided with the same dedication as ANC in developing countries, around 90 percent of maternal deaths that occur during the month after delivery could be avoided.x

A mother arrives at MSF’s Arua Regional Hospital in Uganda for a consultation. Isabel Corthier
MSF staff try to see women twice for postnatal care. The first visit should happen within the first week of the baby’s life if delivery occurred at a medical facility. If the mother gave birth at home, she and the child should ideally be examined within 24 hours. In either case, a midwife or a specially trained nurse checks for danger signs that would indicate medical issues that require immediate attention for the mother. These would include heavy vaginal bleeding, fevers, severe headaches, or hypertension.
At the same time, the midwife checks the baby to see if he or she is breathing and eating well and if there are any signs of jaundice or problems with eyes or umbilicus. Babies usually get Vitamin K during the first visit to help their blood clot. They also get tetracycline eye ointment to protect them from neonatal conjunctivitis, which can cause blindness. Babies should also receive a “birth dose” of vaccinations to prevent tuberculosis, polio, and hepatitis B before they begin routine vaccinations at six weeks old.
If the mother did not receive a tetanus vaccine during ANC, the midwife or nurse will administer it during the first PNC visit, along with vitamin A and ferrous sulfate/folic acid supplements. They’ll talk with the mother about healthy birth spacing, and if she wants contraception, they will provide it.
MSF will also give undernourished mothers supplemental food and HIV-positive mothers antiretroviral treatment, if they are not already receiving it. The staff will also ensure that a baby born to a mother with HIV who is not in a program to prevent transmission gets preventive treatment for HIV. [See Chapter 6: PMTCT]
The benefits PNC brings in the hours and weeks after birth
are numerous, but the challenge is
persuading women to come for the care.
The second visit should come at about six weeks, when the baby starts receiving routine vaccinations. Tying PNC to vaccinations gives women an incentive to receive the care, as most mothers know the value of vaccines and they seem to appreciate receiving both services in one visit. Mothers will have learned about postnatal hygiene, nutrition, and sex, as well as breastfeeding, how to care for the baby, and how to identify potential danger signs in the first visit and these things will be covered again in the second.
Another general benefit of receiving PNC is that the mother and baby may be spared harmful traditional practices. They’ll be warned not to give the baby anything made with water that’s not clean—weak tea, rice water, or diluted animal milk, for instance—which can lead to diarrhea. They should also not allow any unclean substances, such as animal dung or ash, to come into contact with the baby’s umbilical cord at the time of birth.
The benefits PNC brings in the hours and weeks after birth are numerous, but the challenge is persuading women to come for the care. The same measures that MSF health workers employ to draw women to ANC can also work for PNC: they offer basic items like a towel and soap as incentives, and make sure to have extra staff on hand in our projects on market day, when most women are out in the biggest population center in the area and therefore more likely to come in.

A mother receives care from MSF mother-and-child outreach staff in the Sidama Zone of Southern Nations, Nationalities and People’s Region of Ethiopia. Photo by Matthias Steinbach
These days, I work as a specialist advisor on sexual and reproductive health for MSF. Among other duties, I visit projects around the world to help teams improve their services. In 2011, for example, I went to both Pakistan and Bangladesh, where I spent time with two maternity teams that were trying to solve the question of how to get PNC to women in their catchment area. Each came up with a unique solution.
In Kuchlak, an Afghan refugee community in Pakistan’s Balochistan Province, the staff were encouraging women to stay in the birthing unit for at least four hours after delivery so they and newborns could receive preventive care and be monitored for any postnatal issues. This worked well with some women who lived close by the clinic, but many of the patients came from as far as 90 miles (150 km) away. They were the women and the newborns the team was most worried about. They would often arrive in a hired vehicle that waited outside while the mother gave birth, and would leave immediately after. It was highly unlikely that they’d be able to get any PNC in their communities and equally unlikely that they would later make the long journey back to the MSF clinic for follow-up care.
Most women, whether they lived nearby or far away, needed a male attendant in order to leave the house; usually it was their husbands. This was a problem for couples living far away because the man would have to miss a day’s work if his wife stayed at the clinic for treatment and evaluation.
Women often have competing needs,
and the more immediate issues take precedence.
Our staff would hear stories about these patients when a neighbor or relative would come in to get health care and mention what had befallen a new mother in their community. Most of the stories we heard had bad outcomes, and while they could not be considered a scientific measure of what happens to women who do not receive PNC, they were nonetheless important indicators.
To address some of these issues, the team in Kuchlak started providing PNC home visits, when and where possible. A Lady Health Visitor (LHV, a professional position similar to a midwife) would come to a woman’s home during the first and second weeks after delivery. In each visit, the LHV would spend at least 15 minutes with the mother, providing her and her baby with standard PNC and any other treatment that was necessary. The LHV was accompanied by female health educator, who gathered the women in the household and talked to them about vaccinations, breastfeeding, hygiene and other important information. A male health educator spoke to the men of the community about various relevant health issues as well.
This approach proved successful. The LHVs were soon seeing up to 150 women per month. This was in a very volatile region, however, and due to insecurity, the team had to curtail the home visits. They became another casualty of conflict.
MSF has implemented home visits by skilled professionals in other contexts as well, but it’s often not sustainable because sending out staff by vehicle can get prohibitively expensive. A better long-term solution has been training local community health workers to check for danger signs in mothers and babies while also conducting health education sessions. When needed, they can refer patients who need treatment to MSF facilities.
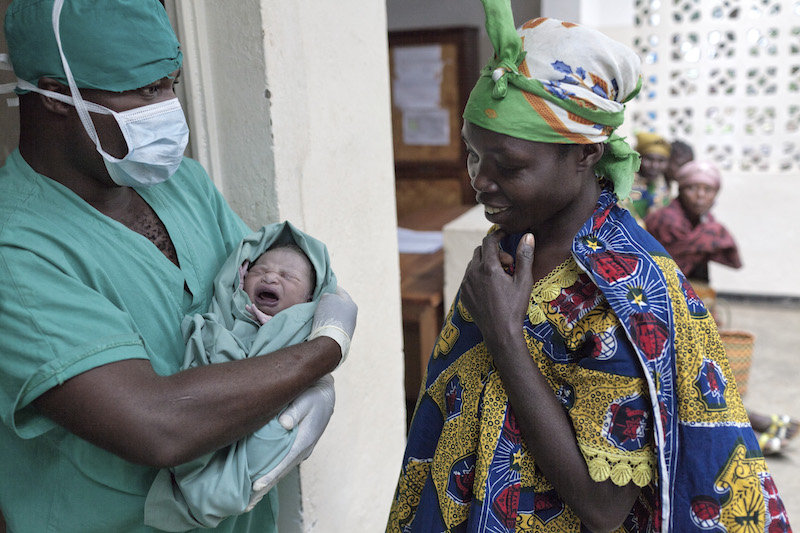
A new mother and father hold their one-day-old baby at the MSF hospital in Masisi, Democratic Republic of Congo. Photo by Yasuyoshi Chiba/Duckrabbit
If a clinic or hospital already offers ANC, very little additional work and expense is required to add PNC. The staff needs are the same, and only a little additional training is necessary. But staff focused on PNC will often encounter the same difficulties faced by those trying to provide ANC. Women often have competing needs, and the more immediate issues take precedence. They may live far from the nearest clinic or hospital and lack money for transport. The roads may be dangerous. They may not be used to seeking preventative care.
The greatest challenge, though, is the lack of awareness about PNC and its benefits. This was starkly evident when I visited the Kutupalong camp in Bangladesh. Kutupalong was an unofficial settlement inhabited by members of the long-ostracized Rohingya ethnic group who had migrated from Myanmar. They were not given any state services and thus had no access to health care. MSF began providing primary medical care on the camp’s outskirts and eventually established a maternity center that offered emergency obstetric care services, ANC and PNC.
When I visited, I was told that many women came in for the ANC component of the reproductive health program but virtually no one was coming for post-partum care. A retrospective study in the camp showed a high incidence of newborn deaths within the first few days of life. The team was making an effort to communicate the importance of PNC in the crucial days after delivery, but there were a host of obstacles that needed to be overcome.
In 2013, MSF staff provided 117,150 postnatal consultations in 116 projects.
This is about one-third of the number of patients who came for ANC.
Nevertheless, the numbers have been slowly increasing over the years.
In Rohingya communities, women often observe a lying-in period of up to six weeks, during which mothers and their babies do not leave the home or do any housework or fieldwork. Naturally, if a woman cannot leave her home, she cannot come in for PNC. Our staff went to the camp’s elders, who are called majees, and explained that the lack of PNC was a primary reason so many newborns were dying. The majees listened and resolved the problem by proclaiming that the MSF clinic could be considered an extension of the women’s homes.
Now, thanks to clear communication, coming to PNC was acceptable. The team just had to figure out how to get new mothers to the clinic.
As a matter of protocol, MSF provides vitamin K and preventive eye treatment to newborns—ideally in the first two days of life, but the medications are effective up to seven days after delivery. The team connected this to their messaging about PNC, casting both as critical aspects of mother and child health that could be provided in the days after a baby was born.
Quickly, we saw that mothers who hadn’t been coming in earlier were now arriving at our clinic seeking both the medications for their newborns and general PNC services. Virtually every new mother in the camp came in for at least one PNC visit within the first few months of the campaign. The numbers later fell and then leveled off at around 40 percent of new mothers—not what it was during the best days, but far better than it was before we started the campaign, and better than the average at most MSF projects.
ANC, skilled delivery, PNC, and newborn care
should be presented as one essential program of care.
While PNC is typically overshadowed by other aspects of maternal care, MSF has increasingly made it an extension of the effort to convince women to seek out skilled assistance during deliveries. More women still seem to respond to offers of ANC, however, as if they believe that once a child is born, there is much less to worry about—even in places where childhood mortality remains a pressing issue. According to the WHO, for instance, PNC programs in sub-Saharan Africa are among the least utilized of all reproductive and child health programs.xi
MSF’s PNC strategy has three main points. First, PNC services need to be promoted during the comparatively well-attended ANC sessions. ANC, skilled delivery, PNC, and newborn care should be presented as one essential program of care.
Second, the message about PNC must also be spread throughout communities. The idea of preventive care should be explained; even if mother and baby are healthy and have no problems, they can still benefit from the service. People in the community also must be made aware of dangers to watch for in mothers and babies.
And third, until all women have access to skilled delivery, MSF staff must establish relationships with traditional birth attendants to improve their referral of women for post-partum care.
With more than 36 percent of maternal deaths occurring during the postnatal period, it’s clear how important PNC is and the impact it can have. It is relatively easy to provide and it gets results. MSF’s data for all projects that offer the service show that in 2013, staff detected illnesses in 11 percent of mothers and 14 percent of babies who were seen for postnatal care. They diagnosed 5,571 women with puerperal sepsis, wound infection, post-partum depression and other illnesses, and 5,420 babies, many with early-onset neonatal sepsis from bad hygienic practices during home deliveries. All were treated and their lives were saved.
This is why MSF sees PNC as a vital service for women and their children, and why we think it is so important to have it be part of the continuum of care—ANC, skilled delivery, PNC and newborn care—that health systems and organizations aspire to provide.
*Patient names have been changed.
iWHO, Global Health Observatory. “Antenatal Care.” Accessed December 2014. http://www.who.int/gho/maternal_health/reproductive_health/antenatal_care_text/en/
iiSereen Thaddeus and Deborah Maine. “Too Far to Walk: Maternal Mortality in Context.” Social Science Medicine, Vol. 38. No. 8, pp. 1091-1110, 1994.http://www.researchgate.net/publication/46505614_Too_far_to_walk_Maternal_mortality_in_context/links/00b495283bb7b3ece3000000
iiiWHO, Essential Medicines and Health Products portal. “Legal Status of Traditional Medicine and Complementary/Alternative Medicine: A Worldwide Review.” 2001. p. 29-30. Accessed December 2014. http://apps.who.int/medicinedocs/pdf/h2943e/h2943e.pdf
ivFrances A. Althaus, “Female Circumcision: Rite of Passage Or Violation of Rights?” Guttmacher Institute. International Family Planning Perspectives. Vol. 23, No. 3, September 1997. http://www.guttmacher.org/pubs/journals/2313097.html
vCarla AbouZahr. Global burden of maternal death and disability, British Medical Bulletin. 2003; 67: p. 7. http://bmb.oxfordjournals.org/content/67/1/1.full.pdf
viNawal M. Nour. An Introduction to Maternal Mortality, Review of Obstetric Gynecology, Spring 2008; 1(2): p. 77–81. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2505173/
viiWHO, Global Health Observatory. Situation and Trends. “Skilled attendants at birth.” Accessed December 2014. http://www.who.int/gho/maternal_health/skilled_care/skilled_birth_attendance_text/en/
viiiUNICEF, “Maternal and Newborn Health.” 2012. http://www.unicef.org/health/index_maternalhealth.html
ixKassebaum et al. “Global, regional, and national levels and causes of maternal mortality during 1990-2013: a systematic analysis for the Global Burden of Disease study 2013.” The Lancet. Vol. 384 No. 9947.pp 980-1004.
xX.F. Li, J.A. Fortney, M. Kotelchuck, L.H. Glover. “The postpartum period: the key to maternal mortality.” International Journal of Gynaecology and Obstetrics 1996;54:1-10.
xiWHO, The Partnership for Maternal, Newborn & Child Health. “Opportunities for Africa’s Newborns: Practical data, policy, and programmatic support for newborn care in Africa.” 2006. p. 79. http://www.who.int/pmnch/media/publications/oanfullreport.pdf